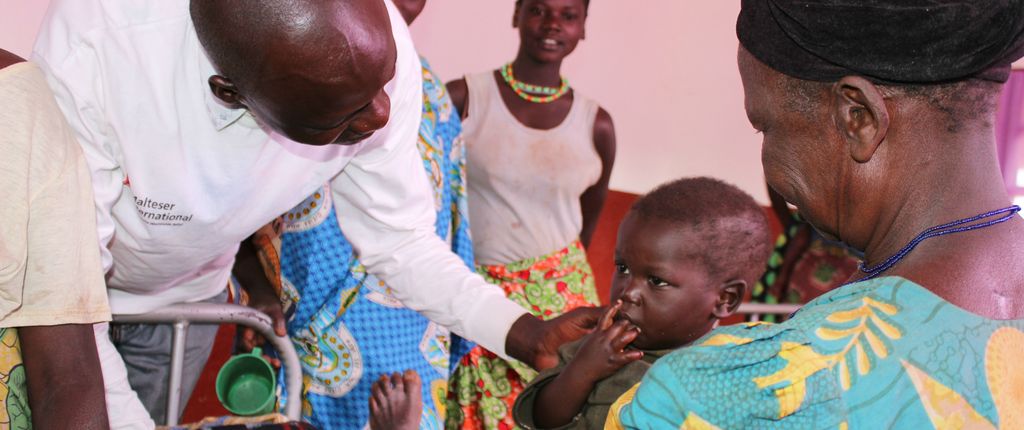
Better health care and nutrition in the border region to the Central African Republic
Since 2013, when the President Bozizé was overthrown, the Central African Republic (CAR) has been in civil war. The armed conflict largely affects the civilian population, which is sometimes even deliberately targeted.
Over 172,000 refugees from the CAR seek protection in the Democratic Republic of Congo. The already critical health care situation in the isolated province of Bas-Uélé in the north of the Democratic Republic of Congo is further intensified by the influx of refugees. A large proportion of the refugees lives within local host families in an out-of-camp context. Due to the ongoing conflict in the CAR, a return of the refugees to their home country is currently out of the question.
Since 2016, we have been working to strengthen the health system in the north of the DRC and to give both the refugees from the CAR and the Congolese host population access to high-quality health care and treatment for malnutrition.
The conflict, originally between the Séléka (an alliance of Muslim rebel groups) and the president's supporters, has become increasingly tensed, with the result that a large number of militias are now fighting for political influence and natural resources. The civilian population suffers heavily from these armed conflicts. After the situation seemed to slowly ease at the end of 2016 and the first refugees returned to the CAR, the conflict has been escalating increasingly since mid-2017, so that many tens of thousands of people have had to seek protection in neighbouring countries. After Cameroon, the DR Congo hosts the largest number of Central African refugees.
Access to the province of Bas-Uélé in the north of the DRC is very difficult due to poor road conditions, destroyed bridges and sometimes a precarious security situation. The local health centres clearly suffer from this poor accessibility. The supply of medicines, for example, is a major challenge for them. Only rarely all the medicines needed for treatment are in stock, and the prices of medicines in the health zone are extremely high due to its remoteness. Many patients can only buy a part of the prescribed medication.
The staff working in the health centres has rarely received formal training, often it is a matter of familiarisation during their daily work. The situation is particularly precarious in the maternity wards, where there is a lack of professionally trained midwives. The technical knowledge of the staff is therefore unfortunately often low, and the quality of the treatments offered is poor. In addition, the health centres and maternity wards are technically inadequately equipped. The condition of the sanitary facilities at the health centres is often very poor. Existing simple pit latrines are quickly filled and replacing them is a financial problem for the health centres.
Similarly, in terms of prevention, early detection and treatment of malnutrition, health personnel and the population often lack technical knowledge and therapeutic feeding is not available. Nutrient-dense food during pregnancy and for children, as well as improved hygiene practices and safe drinking water, are effective means of preventing malnutrition.
Health care workers are often unable to comply with important principles of personal occupational health and infection prevention measures. For example, in the absence of incinerators and waste pits, clinical waste is not properly disposed of and poses a significant safety risk to staff and patients.
The aim of the project is to improve basic health care and the hygiene situation of patients, accompanying persons and staff in the health centres in the north of the province Bas-Uélé (health zones Bondo, Monga and Bili), with special attention to the needs of refugees from CAR. In particular, the supply of acute malnourished children with therapeutic feeding and medicines shall be ensured.
To make this possible, access to and the quality of basic health care for the target group will be improved through a combination of supply with medical drugs and technical equipment, as well as training of health personnel and subsidisation of treatment costs.
The prevention, early detection and treatment of malnutrition will be improved, and the health facilities will be able to locally produce therapeutic feeding.
In addition, the number of infections and the transmission of diseases shall be reduced by implementing measures for infection prevention and improve the hygiene situation of patients, accompanying persons and the staff of the health structures.
- Subsidising treatment costs for patients (partial reimbursement of treatment costs for refugees)
- Training of health care personnel to improve the quality of the medical care and to improve occupational safety
- Training of health personnel in early detection, prevention and treatment of malnutrition, as well as in the local production of nutrient-rich therapeutic feeding (Corn-Soy-Blend), according to national standards
- Reducing the risk of infection by systematically eliminating sources of infection in health care structures and training staff
- Supplying the health centres with medical drugs in the form of adapted kits
- Delivery of necessary medical equipment (including protective equipment for infection prevention)
- Provision of therapeutic feeding to health care facilities
- Construction and equipment of maternity wards at the health centres
- Rehabilitation of operating theatres and laboratories at reference hospitals
- Spring protection to improve water supply for health centres and construction of WASH infrastructure (latrines, shower cabins, incinerators)
- Awareness-raising activities in the communities to promote awareness of the importance of quality health care, especially in the area of mother-child health
Country info
Capital: Kinshasa
Area: 2,345,410 km²
Population: ca. 102.3 million
Project data
Financing: BMZ, German Federal Foreign Office (AA) and donations
Partners: Health centres and referral hospitals, local and national health authorities








